Fibromyalgia And Other Myofacial Pain Syndromes
Fibromyalgia (FMS) is a syndrome characterized by chronic widespread musculoskeletal pain and tenderness, associated with disturbed sleep patterns, chronic fatigue and a spectrum of additional functional symptoms like headaches, mood disturbances such as depression and anxiety.
It need to be differentiated with Chronic Fatigue Syndrome (CFS) which is a clinical syndrome characterized by fatigue lasting over six months which is not associated with physical effort and is not relieved by rest.
In the United States, fibromyalgia affects about 2 percent of people by age 20, which increases to approximately 8 percent of people by age 70 with overall estimated prevalence of around 2-4% in general population. It is predominantly diagnosed in patients between the ages of 20-60 years (mean age 49 years). it is the most common cause of generalized musculoskeletal pain in women between 20 and 55 years. It is more common in women than men with approximately 80% cases being females.

Contributory Factors
Various physical or emotional factors may play a role in triggering symptoms.
Various stressors, including infection, physical or emotional trauma, sleep disturbances, or other medical conditions may play a role.
Positive family history in parents.
More common in women than in men
More common in people not physically active.
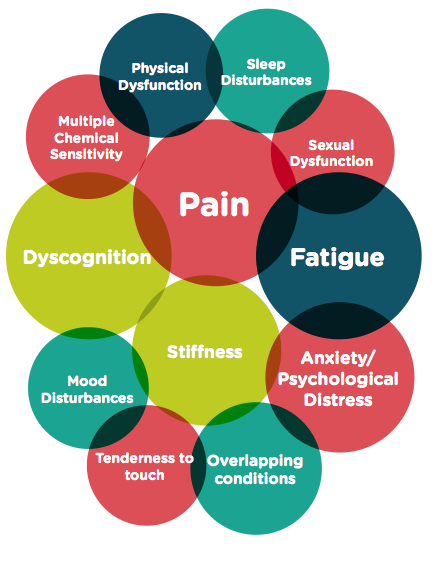
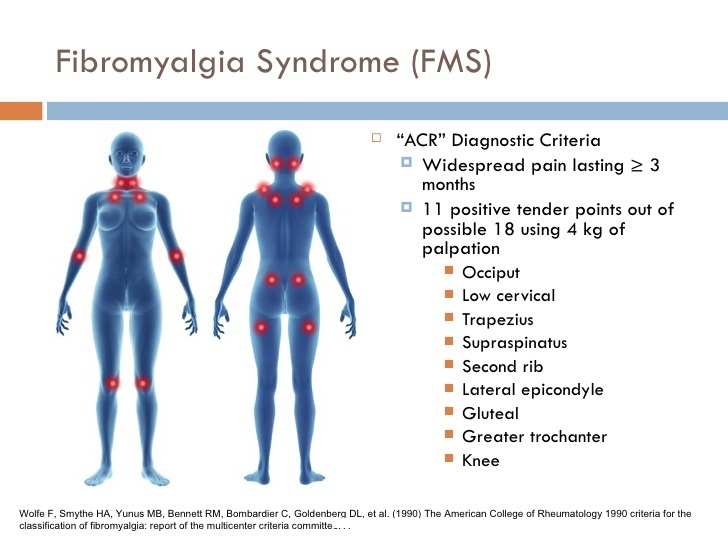
Causes
The cause of fibromyalgia is unknown. Various physical or emotional factors may play a role in triggering symptoms. Although the pain is felt in muscles and soft tissues, there are no visible abnormalities at these sites. The muscles and tendons are excessively irritated by various painful stimuli. This is thought to be the result of a change in pain perception, a phenomenon termed �central sensitization.� Other conditions may also develop as a result of central sensitization, including irritable bowel syndrome (IBS), chronic fatigue syndrome (CFS), chronic headaches, and chronic jaw and facial pain. The most plausible theory suggests that some people have a genetic predisposition to fibromyalgia because of a heightened sense of pain. In other people, various stressors, including infection, physical or emotional trauma, sleep disturbances, or other medical conditions allow for the development of fibromyalgia . The chance of developing fibromyalgia is increased eightfold in family members of a person with fibromyalgia compared with people in the general population. Similar genetic factors are noted in people with irritable bowel syndrome, depression, and migraines.
Treatment
Optimal treatment of fibromyalgia should include the patient, clinician, physical therapist, mental health professional, and other healthcare professionals. General advice should include the following: Fibromyalgia is not a degenerative or deforming condition, nor does it result in life-threatening complications. However, treatment of chronic pain and fatigue is challenging, and there are no �quick cures.� Treatments are available. Medications may be helpful in alleviating pain, improving the quality of sleep, and improving the mood. Exercise, stretching programs, and other activities are also important in helping to manage symptoms. Symptoms of fibromyalgia are not related to any destructive process, and being active will not cause harm.
FIBROMYALGIA MEDICATIONS :
As of 2011, three medications had been approved by the FDA for the treatment of fibromyalgia. These included pregabalin, an alpha-2-ligand inhibitor, SNRIs like duloxetine and TCAs like amitriptyline.
Anticonvulsants
Anticonvulsants (drugs used primarily for treating epilepsy) may help to relieve pain and improve sleep. Pregabalin was the first drug approved in the United States for the treatment of fibromyalgia in 2007
Dual-reuptake inhibitors
Duloxetine and milnacipran, both inhibitors of norepinephrine and serotonin reuptake by nerve cells, have helped pain, fatigue, and well-being in people with fibromyalgia, regardless of whether or not the person was depressed . The most common side effects of these dual reuptake inhibitors are nausea and dizziness, but these are generally less problematic if the dose is started at a low level and is increased very slowly.
Tricyclic antidepressants (TCAs)
Taking TCAs before bedtime may promote deeper sleep and may alleviate muscle pain. Examples of TCAs include amitriptyline or cyclobenzaprine.
Analgesics
Analgesics are pain medications; some are available over-the-counter while others require a prescription. The prescription analgesic tramadol, either alone or combined with acetaminophen, was found to be helpful in alleviating the pain associated with fibromyalgia in clinical trials. Tramadol may cause dizziness, diarrhea, or sleep disturbances in some people. Use of tramadol is less likely to result in addiction compared with other, more potent narcotic pain relievers.
Exercise
Regular cardiovascular exercises, such as walking, swimming, or biking, are helpful in reducing muscle pain and improving muscle strength and fitness in fibromyalgia. Muscle strengthening programs also appear to improve pain, decrease the number of tender points, and improve muscle strength in people with fibromyalgia. People with fibromyalgia should consider working with a physical therapist to develop an appropriate, individualized exercise program that provides the greatest benefit. Eventually, a person should exercise for a minimum of 30 minutes three times weekly.
Types of Pain
- Neck Pain
- Low Back Pain
- Thoracic Spine Pain
- Headache
- Shoulder Pain
- Elbow Pain
- Wrist Pain
- Knee Pain
- Peripheral Vascular Disease
- Neuropathic Pain Syndromes
- Fibromyalgia And Other Myofacial Pain Syndromes
- Chronic Regional Pain Syndrome
- Facial Pain
- Foot Pain
- Abdominal Wall Pain Syndrome
- Sacroiliac Joint Pain
- Cancer Pain
- Urogenital Pain Syndrome
- Chronic Pelvic Pain