Chronic Regional Pain Syndrome
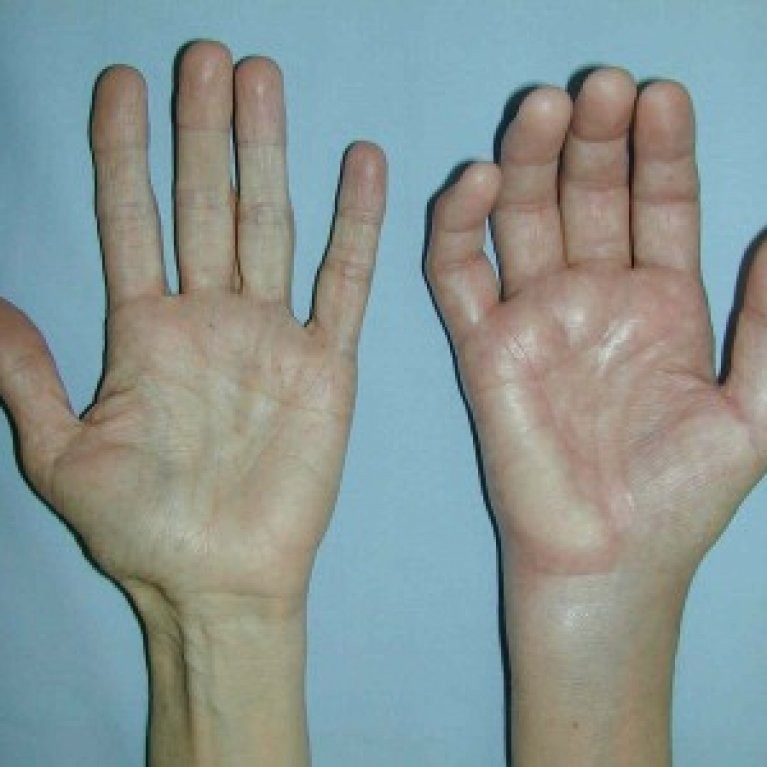
Complex regional pain syndrome (CRPS) is a chronic (lasting greater than three months) pain condition that most often affects one limb (arm, leg, hand, or foot) usually after an injury. The pain is usually triggered by some injury or trauma. It is caused by malfunction or damage to the central or the peripheral nervous system. The damaged nerves are not able to properly control the blood flow and hence causing pain and other problems. CRPS has also been reported as a complication of minor surgical procedures. In addition, the syndrome has been reported following nerve injury caused by intramuscular injection or routine venipuncture and as an adverse reaction to subcutaneous allergic reaction. It is also sometimes associated with medical conditions such as diabetic neuropathy, multiple sclerosis, myocardial infarction and cancerous infiltration of a nerve plexus.
Contributory Factors
Thought to be caused by an injury to or an abnormality of the peripheral and central nervous system. Female sex, Rheumatoid arthritis, accompanying ulnar fracture, open fracture, and open reduction were identified as significant risk factors for CRPS-1.
Also high energy trauma, severe fracture, strong pain after fracture, decreased sympathetic vasoconstrictor response after fracture, nerve and spinal cord injury, ankle dislocation, ankle fracture, injury in the extremities, motor nerve injury, decreased function before operation, poor physical functioning, social or psychological stress, osteoporosis, hypertriglyceridemia, rheumatoid arthritis, musculoskeletal comorbidities, history of allergies, skin hypersensitivity, atopic background, asthma, trouble falling asleep, menstrual cycle related problems, history of CRPS I, chronic pain, headache/migraine, first-degree family history of headache, fibromyalgia, multiple sclerosis are reported to be a risk factor for CRPS
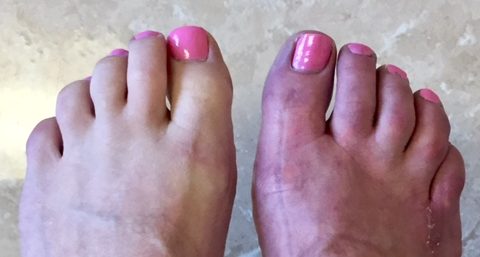
Investigation
Laboratory Studies
- No specific diagnostic tests confirm the presence of CRPS. However, the differential diagnosis includes other neuropathic conditions, as well as a host of metabolic, systemic, vascular, and rheumatological disorders. Excluding other treatable but serious causes is indicated even in cases that present with the classic signs and symptoms.
- Blood work for inflammatory arthropathy and vasculitis is indicated, which, in its basic form, includes complete blood count (CBC), erythrocyte sedimentation rate, C-reactive protein, antinuclear antibody, rheumatoid factor, complement fixation panel, serum immunoelectrophoresis, and a bone scan. Workup for diabetes should also include a test for hemoglobin A1c.
- Electromyography (EMG) and nerve conduction studies are helpful in determining the neuroanatomy behind the symptoms and therefore in identifying the etiological process. For example, they confirm the presence of nerve injury, CRPS type II, nerve root avulsion, or a painful neuropathy due to diabetes, which may present with autonomic dysfunction.
- Vascular studies of the affected limb(s) should also be considered.
Imaging Studies
- Osseous changes are common in CRPS; therefore, most standard diagnostic test results used to support or refute clinical evidence for this diagnosis demonstrate changes, or a lack thereof, in the bones and joints.
- Radiography: In the chronic stages of CRPS, plain radiographs may reveal endosteal and intracortical excavation, resorption of subperiosteal and trabecular bone, localized bone demineralization, and/or osteoporosis.
- Bone scintigraphy: Compared with radiography, 3-phase bone scintigraphy has higher sensitivity (97% vs 73%) and specificity (86% vs 57%) in early post fracture CRPS.
- 3-phase bone scintigraphy can provide valuable information during the first year and is useful in differentiating CRPS from other pain syndromes. Homogeneous unilateral hypoperfusion in the perfusion and blood-pool phases is considered characteristic of CRPS and repudiates osteoporosis due to inactivity. These 2 initial phases are seen at 30 seconds and 2 minutes postinjection, respectively. At 3 hours postinjection, the mineralization phase shows increased unilateral periarticular uptake. This pathological uptake is thought to be highly sensitive and specific to CRPS. On the other hand, scintigraphy only shows significant changes during the first year. Additionally, this test is less valuable in children than in adults due to its higher variability.
- Magnetic resonance imaging (MRI): MRI scans have demonstrated changes in joints (joint effusion) and soft tissues with CRPS with high sensitivity but less specificity.
Treatment
Pharmacological agents:
- Tricyclic antidepressants: The drugs commonly used are amitriptyline, nortriptyline.
- Anticonvulsants like gabapentin may give some relief.
- Clonidine: It works by stimulating inhibitory descending inhibitory pain pathways that are norepinephrine dependent.
- NMDA receptor antagonists like ketamine and methadone may be tried.
- Baclofen having role on descending inhibitory pathway may be tried.
- Opioids like tramadol or combinations with paracetamol may be tried to control pain.
- Bisphosphonates
- Steroids may be useful in early stages of CRPS
Types of Pain
- Neck Pain
- Low Back Pain
- Thoracic Spine Pain
- Headache
- Shoulder Pain
- Elbow Pain
- Wrist Pain
- Knee Pain
- Peripheral Vascular Disease
- Neuropathic Pain Syndromes
- Fibromyalgia And Other Myofacial Pain Syndromes
- Chronic Regional Pain Syndrome
- Facial Pain
- Foot Pain
- Abdominal Wall Pain Syndrome
- Sacroiliac Joint Pain
- Cancer Pain
- Urogenital Pain Syndrome
- Chronic Pelvic Pain